|
The
length of hospital stay of Home Health Care patients
at King Khalid National Guard Hospital, Jeddah, 1999.
|
|
Authors
Nisreen A. Jastaniah , Fahad Al-Tayyeb , Bakar Bin Sadeq.

Abstract
Objectives: This study was initiated
to identify diseases followed by Home Health Care (HHC) Team
at King Khaled National Guard Hospital (KKNGH), and to compare
the length of hospital stay, the number of outpatient and
emergency room visits in patients receiving Home Health Care
to those who do not get this service over a 6-month to one
year period.
Design: This
is a cross sectional study to identifying diseases followed
by Home Health Care Team and case control study for the follow
up of patients.
Setting and Participants:
Home health care at King Khaled National Guard in
Jeddah . All patients followed by the HHC team on February
2000 were included. The same numbers of patients with the
most frequent diagnosis were admitted before 1997(non-HHC.
Measurements: demographic
data for HHC patients, and type of care patients needed .
The second objective, total in-patients days, number of emergency
,and clinic visits for six month to one year for HHC patient
,and non-HHC patients.
Results: There were148
patients, 83 (56.1%) male, And 65 (43.9%) female with mean
age of 47.4-year rang 6 month- 99 years. There was 111 (75%)
adult (above 18 years) with mean age of 61.2 years range between
20 years -99 years. 37 (25%) pediatrics patients found with
mean age of 7.3 years range 6-month -18 years. Among the 148
patients 30 (20.3%) were found to have circulatory system
disorder, mainly stroke (CVA (29). Twenty four patients (16.2%)
diagnosed as having nepotistic disease, 13 (8.8%) patients
with injuries, 10.8% with endocrine disorders mainly diabetes
and the rest were with other disorders . About 25.7% of these
patients have one more diagnosis. Ninety-three (62.8%) of
HHC patients needed continuous care (chronic care), 23 (15.5%)
were for palliative care, 18 (12.2%) needed transient care
i.e. health education and flow up, while 14 (9.5%) needed
acute care after discharge from hospital. The mean hospital
stay days were 14.9 days for HHC CVA cases at the first admission,
while it was 10.6 days for hospital CVA cases who did not
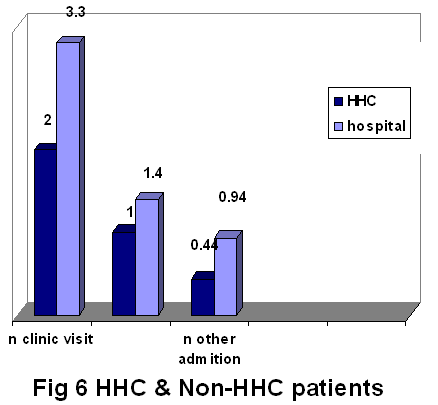
have HHC service (P value 0.226).The mean number readmission
was lower for HHC patients than for non-HHC CVA (0.44 admission,
0.94 admission) respectively(P value 0.116). HHC patient means
clinic visits during 6month to 1 year was 2, while it was
3.3 for hospital CVA patients. This difference has no statistical
significance (p value 0.127).
The emergency means visits during 6month -1 year for HHC cases
was 1, on the other hand it was 1.4 for the hospital patients.
This also had no statistical difference (P value 0.325).
Conclusion: Home
health care at King Khaled National Guard in Jeddah is covering
different age groups with a variety of diagnosis. The most
common one was CVA. Some patients have more than one diagnosis,
and have some complex medical and social condition, that needed
more than one service (nursing, physiotherapy, social support,
equipment,) these patients needed care for a longer period
of time with frequent visits per week. HHC also provides palliative
care for terminal illnesses and acute care for post hospital
discharge.The hospital readmission's, clinic visits, and emergency
visits were lower in HHC patients than non-HHC however this
difference was not statistically significant.
Abbreviations:
| HHC |
Home Health Care. KFNGH King Fahad National Guard hospital |
| KKNGH |
King Khaled National Guard
Hospital |
| Non-HHC patients |
Patients, who did not have
HHC services |
| CVA |
Cerbrovascular Accident |
| DM |
Diabetes Maltese |
| HPN |
Hypertension |

Introduction
Home Health Care (HHC) is a formal, regulated program of care
delivered by variety of health care professionals in the patient
home. [1] HHC services are provided by physicians, nurses,
physio-therapists, occupational therapists, speech therapists,
home care aids, social worker, and dieticians; as well as
drug and equipment supply [2].
For the last fifty years home visits started
to decline. Some of the major reasons were due to: the advancement
of medical technology; a wide spread of the telephone and
communication technology enabled the physician to give over
the phone advice and to receive follow up information more
readily [3]. Lack of practice and experience in caring for
patients at home, medical literature concerning HHC are very
few to none; and the financial factor (since payment for HHC
is considerably less than in clinics for the same amount of
time [4].
On the other hand many reasons have helped home visits to
start again and to be considered as one of the fastest growing
Medicare sector. This change could be because the in-patient
model of care may not be optimally serving the needs of the
growing number of elderly and disabled people [2]. The comfortable
home environment makes patients choose to receive care at
home. It makes them feel a greater sense of well being which
helps in improving their participation in the management of
their care [5].
Home Health Care in Saudi Arabia
In the Kingdom of Saudi Arabia Home Health Care services was
started by the Green Crescent Hospital in 1980, as a part
of their emergency program. [6] King Faisal Specialist Hospital
and Research Center implemented HHC service in 1991 under
the supervision of a committee to oversee its ongoing planning
and implementation, following a pilot study which indicated
that patients and their families benefited from the nursing
care and psychosocial support. The study demonstrated that
such a program reduced the need for hospital admissions, clinic,
as well as the number of emergency visits. [7]
King Fahad National Guard Hospital (KFNGH) in
Riyadh started Home Health Care in spring 1995 [6]. It covers
all patients referred from KFNGH according to their selection
criteria. Home care services started on 1997 in the National
Guard Hospital. H. H. R. Princess Hussa Bint Trad Al-Shaalan
officially opened it on April 29th 1998 under the supervision
of H. R. H. princes Adellah bent Abdullaa bin Abdulazeez.
The service covers all patients who are eligible to be treated
in National Guard Hospital who are home bound, need medical
services, and are 50 kilometers away from the hospital. It
provides nursing, social service, physiotherapy, respiratory
therapy, dietary, psychotherapy, medications, and equipment
supply according to the patients needs.
Home care and family medicine
Primary care physicians developed a sustained partnership
with their patients by providing an integrated, accessible
health care service, practicing in the context of family and
community, and addressing patient's health care needs (9).
So Primary care is the comprehensive management of unselected
patients with undifferentiated problems. (9)
The primary care doctor is responsible for the
biopsychsocial model in managing his patients and need to
evaluate the environmental conditions. One study found that
home assessment of elderly patients with relatively good health
status and function resulted in the detection of an average
of four new medical problems and up to eight new intervention
recommendations per patient. (10). The major problems detected
included impotence, gait and balance problems, immunization
deficits, and hypertension. Significantly, these problems
had not been expected based on information obtained from outpatient
clinic encounters (11). Specific home-based interventions,
such as adjusting the elderly patient's home environment to
prevent falls, have also yielded health benefits. (12)
Home care is a way a family physician can conduct
follow up visits with patients with chronic illnesses. It
allows the physician to assess other factors not readily seen
in hospital visits (like the home environment) which may have
a big effect on the condition and treatment of the patient.
This type of care can help bring a better understanding between
patient and doctor and can lead to better cooperation and
management of the patient.
Type of visits
The following are the different types of home visits:
Illness home visits; The illness home visit
involves an assessment of the patient and the provision of
care in the setting of acute or chronic illness, often in
coordination with one or more home health agencies. Emergency
illness visits are infrequent and impractical for the typical
office-based physician.(12)
Dying patient home visits; The dying
patient home visit is made to provide care to the home-bound
patient who has a terminal disease, usually in coordination
with a hospice agency. The family physician can provide valuable
medical and emotional support to family members before, during,
and after the death of a patient in the home environment.
(12)
Assessment home visits;: The assessment home
visit can also be described as an investigational visit during
which the physician evaluates the role of the home environment
in the patient's health status. An assessment visit is often
made when a patient is suspected of poor compliance or has
been making excessive use of health care resources. Medication
use can be evaluated in the patient who is taking many drugs
(polypharmacy) because of multiple medical problems. Evaluation
of the home environment of the "at-risk" patient
can reveal evidence of abuse, neglect or social isolation.
A joint assessment home visit facilitates coordination of
the efforts of home health agencies and the physician. (12)
Hospitalization follow-up home visits; Follow-up
home visits after a patient has been hospitalized are very
useful when significant life changes have occurred. For example,
a home visit after the birth of a new baby provides an excellent
opportunity to discuss wellness and prevention issues and
to address parental concerns. A home visit after a major illness
or surgery can be useful in evaluating the coping behaviors
of the patient and family members, as well as the effectiveness
of the home health care plan. (12)
Home care and clinical pathway
Developing a clinical pathway is an important issue to evaluate
and can give measurable out come (13). It also can help in
following the patients with multiple medical problems. So
many pathway models are used to asses multiple and different
issues. One of these models is the INHOME mnemonic, which
was devised to help family physicians to remember the items
to be assessed during home visits. This model is directed
at a patient's functional status and living environment. This
mnemonic can be expanded to "INHOMESSS," which incorporates
investigations of safety issues, spiritual health and home
health agencies (12).
The" INHOMESSS" Mnemonic stands
for; I =Immobility ,N =Nutrition ,H =Housing ,O =Other
people ,M =Medications ,E =Estimations
S =Services by Home Health Agencies ,S =Spiritual Health and,S
=Safety.
Immobility: Evaluation of the patient's functional
activities includes assessment of the activities of daily
living (bathing, transfer, dressing, toiling, feeding, continence)
and the instrumental activities of daily living (using the
telephone, administering medications, paying bills, shopping
for food, preparing meals, doing housework). The physician
can ask the patient to demonstrate elements of the daily routine,
such as getting out of bed, performing personal hygiene and
leisure activities, and getting in and out of a car. (12)
Nutrition: The physician should assess the patient's
current state of nutrition, eating behaviors, and food preferences.
Healthy food preparation techniques can also be reviewed with
the patient. (12)
Home Environment: The patient's home environment
should allow for privacy, social interaction, spiritual and
emotional comfort, and safety. A safe neighborhood within
close proximity to services is important for many older patients.
(12)
Other People: Having the patient's social support
system present at the home visit clarifies the roles and concerns
of family members. During routine visits, the physician can
assess the availability of emergency help for the patient
from family members and friends and can clarify specific issues,
such as who is to serve as surrogate for the patient in the
event of incapacitation. Evaluation of the caregiver's needs
and risk of burnout is critically important. (12)
Medications: To remedy or avoid polypharmacy,
the physician must evaluate the type, amount and frequency
of medications, and the organization and methods of medication
delivery. An inventory of the patient's medicine cabinet can
provide clues to previously unidentified drug-drug or drug-food
interactions. A home medication review can also allow a direct
estimate of patient compliance. (4)
Examination: The home visit should include a
directed physical examination based on the needs of the patient
and the physician's agenda. Practical, function-related examination.
The physician can have the patient demonstrate proper technique
for the self-monitoring of blood glucose levels. In addition,
the physician can weigh the patient and obtain a blood pressure
measurement. In-person correlations of home and office measures
provide useful information for future telephone and clinic
contacts. (12)
Safety: The goal of the home safety assessment
is to determine whether the patient's environment is comfortable
and safe (no unreasonable risk of injury). To raise the subject,
the physician should simply state the intention to identify
and help modify potential safety hazards. (12)
Studies done on home health care
Studies showed that a group of elderly under 24 hours home
care demonstrated better instrumental activities of daily
living, out door walking and significantly fewer diagnosis
and drugs at 6 months. They used fewer in-patients and more
out patient care than the control group. Also significant
cost reduction was found in the home care group (14). Another
study on home health showed that nurses conducted 70% of all
home visits (15). A study found that patients with hip fracture
who were under HHC (after discharge from hospital) had lower
hospital readmission for one year (16). It concludes that
there is a relative effectiveness of post acute service and
post discharge (16). Another Study described the management
of patients at home after prostatectomy is an excellent example
in which patients who received home care had the same outcome
and frequency of readmission as those discharged from hospital
2 or 3 days later. (17)
On the other hand Cochrane Library reviewed
11 RCS studies and concluded; that there is insufficient evidence
to assess the effects of hospital-at-home on patient outcomes
or the cost to the health service. Given the heterogeneity
of what hospital-at-home encompasses and the uncertainty over
its effects, future research should clearly specify the type
of service being provided, both at home and at hospital, and
the specific patient groups. Patient health outcomes, patient
and carrier satisfaction, and costs should be measured, and
studies should include a formal, planned economic analysis.
Studies should be large enough to detect important differences
and to ensure generalisability of the result (18).
Rationale
Home Health Care helps the physician to fully understand the
social factors related to his patient. This understanding
will assist the physician in patient management as well as
strengthen the patient-doctor relationship. From my knowledge
very few studies were carried out locally on HHC [7] despite
its importance, so this study may help in bridging this gap.
Aim
The aim of this study is to determine the effectiveness of
the Home Health Care program at King Khalid National Guard
Hospital (KKNGH).
Objectives
The objectives of this study are:
1. To identify the different diseases followed by the Home
Health Care Team at KKNGH and to determine the most frequent
diseases.
2. To compare the length of hospital stay, the number of outpatients
and emergency room visits with Home Health Care services in
the treatment of the same frequent diseases. This was to be
done within a 6-month period or more depending on case of
study.
Area profile
The city of Jeddah is located in the western region of Saudi
Arabia and borders the eastern coast of the Red Sea. Jeddah
is nearly 580 square kilometres, and it population is around
2 million. [8] The Ministry of Health, Military, National
Guard, Private hospitals and Primary Health Care Centres cover
the medical services in the city. The research in this study
will be carried out in the Home Health Care Centre, at King
abdulazeez medical city .Um Al Salam area, Jeddah.
Methodology
Preparatory phase: Following a considerable
review of the literature, the researcher prepared a preliminary
checklist. After the research proposal was formally accepted,
the preset checklist was tested on a sample of records. The
checklist was modified, following this small pilot study.
Type of the study: This is a cross
sectional study for the first objective, and case control
study for the second objective.
Patients and data collection
Data was collected for All patients followed by the HHC team
on February 2000. All these patients were eligible for treatment
in the National Guard Hospital. All were Saudi patients (the
first check list was used for that). Patient name, mrn, age,
sex, referring department, type of care i.e. (transitional
-for limited time-, acute for evaluation, palliative for advanced
cancer and terminal illness and chronic for those who need
long time flow up), and services provided i.e. (nursing, social,
equipment, physiotherapy, respiratory therapy, dietary, and
psychotherapy). Data entered into the computer for analysis
was done using the SPSS program.
The same numbers of patients with the most frequent
disease were admitted before 1997(non-HHC). Data was taken
from the hospital records for comparing the length of stay
during the first admission, the number of subsequent admissions
and number of both emergency and clinic visits for 6 month
to one-year time.
Tools of the study
Two checklists used (appendixes 1, 2). The first list included
the following variables; patient name, MRN, age, gender, diagnosis,
and the type of care given for HHC patients. The second list
included; patient name, age, gender, diagnosis, and total
in-patients days, and number of emergency and clinic visits
for one year to six months. A Copy of both lists will be submitted
in the appendix.
Case Selection Criteria
All Saudi patients, male and female with the most frequent
diagnosis for flow up and under the care of the HHC department
at KKNG Hospital during February 2000 have been included in
this study. They were followed for at least a period of 6
months. Control Selection Criteria:
The following are the selection criteria for
the control (non-HHC patients) who were included in the study:
· must be Saudi patient
· they must have the same diagnosis as the case patient
· never had HHC service
· They were treated at KKNG hospital before 1997(before
the implementation of HHC).
· The numbers of control were equal to the number of
cases.
Data Analysis
The researcher entered all data to the SPSS program on a personal
computer. Statistical analysis was done using the SPSS program.
Chiseqare, T. test, anova and other tests were used for data
analysis. A p-value of 0.05 or less was taken as statistically
significant in the final data analysis and confidence interval
of 95%. To insure correct data entry, all entered records
were rechecked.
Ethical Consideration
- Letter from the main supervisor of the Joint Program of
the Family and Community Medicine for KKNG Health Affairs.
- All information in the file will be kept confidential.
Results
Sample size: The total number of patients
under HHC during February 2000 was 148 patients. The most
frequent diagnosis was cerbrovascular accident (CVA) 30 patients
(20.3%). Sixteen patients who had follow up for more than
6 month were compared with 16 non-HHC CVA patients.
Age & gender: There
were 83 (56.1%) male. And 65 (43.9%) female with mean age of
47.4-year rang 6 month- 99 years. Among the 148 patients there
was 111 (75%) adult (above 18 years) with mean age of 61.2 years
range between 20 years -99 years. 37 (25%) pediatrics patients
found with mean age of 7.3 years range 6-month -18 years.
Table 1:
Distribution of sex by age-group
| AGE
GROUPS |
SEX |
TOTAL |
|
Male
(%)
|
Female
(%)
|
|
0 -
4
|
8 (5%)
|
5 (3.4%)
|
13
(8.8%) |
5 -
14
|
10
(6.8%)
|
10
(6.8%)
|
20
(13.6%) |
15
- 40
|
14
(9.5%)
|
9 (6.1%)
|
23
(15.6%) |
41
- 65
|
18
(12.2%)
|
21
(14.2%)
|
39
(26.4%) |
| >
65 |
33
(22.3%)
|
20
(13.5%)
|
53
(35.8%) |
| Total |
83
(56.1%) |
65
(43.9%) |
148
(100%) |
|
Diagnosis:
Among the 148 patients 30 (20.3%) were found
to have circulatory system disorder, mainly stroke (CVA (29).
Twenty four patients (16.2%) diagnosed as having nepotistic
disease, 13 (8.8%) patients with injuries, 10.8% with endocrine
disorders mainly diabetes and the rest were with other disorders
like central nerves system disorders, dermatological, genitourinary,
and bone diseases (Table 2). About 23 (15.5%) of patients
were pediatric, suffering from mental retardation and other
syndromes. About 25.7% of these patients have one more diagnosis
i.e. diabetes or hypertension. Nine point five percent have
two or more other diagnoses.
Table 2:
Distribution of HHC patients' diagnosis by gender
| Diagnosis
Category |
SEX |
TOTAL |
|
Male
(%)
|
Female
(%)
|
|
Circulatory
disorder
|
20
(66.7%)
|
10
(33.3%)
|
30
(20.3%) |
Neoplasm's
|
11
(45.8%)
|
13
(54.2%)
|
24
(16.2%)
|
Injuries
|
11
(84.6%)
|
2
(15.4%)
|
13
(8.8%) |
Endocrine
disorder
|
8
(50%)
|
8
(50%)
|
16
(10.8%) |
Pediatric
diseases
|
14
(60.9%)
|
9
(39.1%)
|
23
(15.5%) |
Others
|
19
(45.2%)
|
23
(54.8%)
|
42
(28.4%) |
| Total |
83
(56.1%) |
65
(43.9%) |
148
(100% |
|
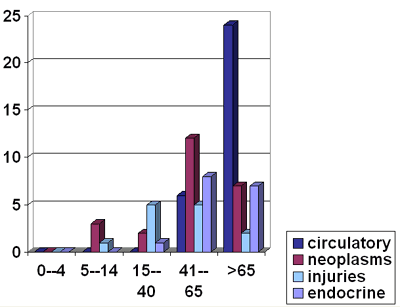
Age &
diagnosis: Out of the 30 cases that have circulatory
system disorders 24(80%) were in the age group of more than
65 years. Neoplasms were more common in the age group from
41-65 years 12 (50%). Injuries were found to be more common
in the age groups 15-65 years
Fig 2: Age
& diagnosis
Type of
care: Ninety-three (62.8%)
of HHC patients needed continuous care (chronic care), 23
(15.5%) were for palliative care, 18 (12.2%) needed transient
care i.e. health education and flow up, while 14 (9.5%) needed
acute care after discharge from hospital. (Table 3 Type of
care with diagnosis).
Table 3: Diagnosis &
type of care
| Type
of Care |
Diagnosis
|
Acute
|
Chronic
|
Palliative |
Transient
|
Total |
Circulatory
|
2
|
24
|
|
4
|
30 |
Neoplasm
|
1 |
1
|
18
|
4
|
24 |
Injuries
|
|
10
|
1
|
2 |
13 |
Endocrine
|
3
|
12
|
1
|
|
16 |
Pediatric
|
2
|
18
|
1
|
2
|
23 |
Others
|
6
|
28
|
2
|
6
|
42 |
| Total |
14
(19.5%) |
93
(62.8%) |
23
(15.5%) |
18(12/2%) |
148
(100%) |
|
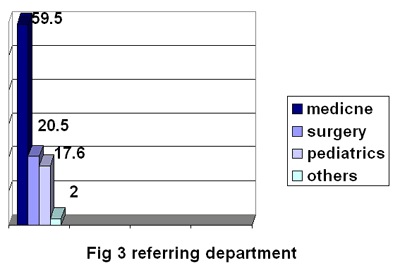
Referring department: Eighty-eight
patients (59.5%) referred from medical departments, 31 patients
(20.5%) surgical referrals, 26 patients (17.6%) from pediatrics
departments, and 3 patients (2%) from other departments. Thus
showed that there was significant difference between medical
department and other referring departments.
There was no statistical
difference among surgical patients and medical department
patients by age (T test .99, df 117, P value 0.32). Also there
were no statistical differences by the number of services
provided to patients and the referring departments (F test
2.2, P value of 0.1).
Fig 3
Service given:
Out of 148 patients, 137 (92%) needed nursing care. This was
the most frequent type of service provided to the HHC cases.
About 68 (45.9%) of the patients needed physiotherapy. Social
support, and evaluation given to 43 (29%) of the patients.
About 25 (17%) patients needed equipment. Nutritional advice
and supplements provided for 33 (22.3%) patient's, 10 (6.8%)
patients needed respiratory therapy, 8 (5.4 %) patients were
given occupational therapy to help them to restore their normal
daily function, and only 4 (2.7%) patients needed psychotherapy.
(Table 4)
Sixty-seven percent of the
patients needed one, or two services. The rest 33% needed
more than 2 services. There was no statistical difference
between age.
Table 4: Services given
to patients
Service
|
Patients
(%)
|
Service
|
Patients
(%) |
Nursing
|
137
(92)
|
Nutritional
|
33
(22.3) |
Physiotherapy
|
68
(45.9)
|
Respiratory
|
10
(6.8) |
Social
|
43
(29)
|
Occupation
|
8
(5.4) |
| Equipment |
25
(17) |
Psychotherapy |
4
(2.7) |
|
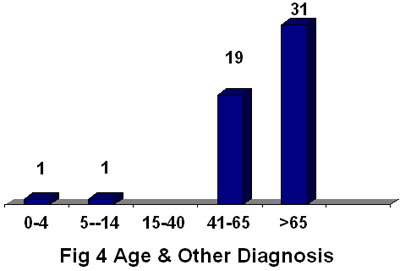
Age & number of other diagnosis:
Age was correlated to the number of diagnosis other than the
main diagnosis for which the patients were being followed.
One or more diagnosis found in 19 (48.7%) of cases from 41-65
years, also it was 31 (58.5%) of patients more than 65years.
There was an association between age group and the presence
of other diagnosis. As the patients age increased patients
had one or more other diagnosis (chi- square 39.6, df 4, P
value 0.01.
HHC and non-HHC patients:
Sixteen patients of HHC clients with CVA who were
followed for more than 6 months were selected for comparing
the length of hospital stay, other admission days, clinic
visits, and emergency visit numbers with 16 non-HHC CVA patients.
Among HHC CVA cases there were 11 males and 5 females with
mean age of 79.9 years Std +, - 11.9. The non-HHC cases were
16 patients who had CVA before 1997 (8 males and 8 females)
with mean age 76.2 Std +, - 5.3. There was no statistical
difference in age of both HHC & non-HHC patients (T test
1.6, df 30, P value 0.13), and in sex (Chi-square 1.1, df
1, P value 0.28). There was also no statistical difference
in the number of other diagnosis in both groups (Chi-square
1.1,df 1, P value 0.28). Table 5.
Table 5: Comparison of HHC & Non-HHC CVA cases
HHC
& non-HHC CVA
|
Statistical test
|
P value |
Age
|
T
test = 1.6
|
0.13 |
Gender
|
Chi-sq.
= 1.1
|
0.28 |
| Other
diagnoses Number |
Chi-sq.
= 2.7 |
0.43 |
|
Hospital stays & number
of re-admission: The mean hospital stay days were
14.9 days for HHC CVA cases at the first admission, while
it was 10.6 days for hospital CVA cases who did not have HHC
service. But there was no statistical significance (T test
1.2, df 30, P value 0.226). The mean number readmission was
lower for HHC patients than for non-HHC CVA (0.44 admission,
0.94 admission) respectively. This difference was not of statistical
significance (T test 1.6, df 30, P value 0.116). There was
no statistical difference in the total of other admissions
days (T test 1.09, df 30, P value 0.282).
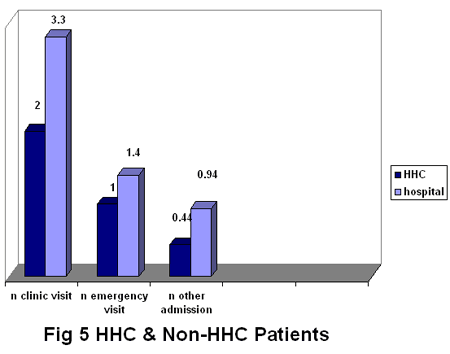
Number of clinic & emergency visits:
HHC patient means clinic visits during 6month to 1 year was
2, while it was 3.3 for hospital CVA patients. This difference
showed no statistical significance (T test 1.57, df 30, p
value 0.127). The emergency means visits during 6month -1
year for HHC cases was 1, on the other hand it was 1.4 for
the hospital patients. This also had no statistical difference
(T test 1, df 30, P value 0.325).
Figure 5
.
Discussion
Home care is an important health service, which deals
with patients in their home environment, and the sharing in
their management. It has many advantages for both the patients
and health services.
The Ages in this study ranged from 6 months
to 99 years, with a mean of 47 years and a median of 56.5
years. This is lower than what was reported in studies done
in Nebraska, New Jersey, and Wisconsin. In these studies the
age of HHC patients ranged from birth to 104 years with a
median of 68.6 years. (18) This difference maybe due to longer
life expectancy in the western community and larger number
of elderly.
Male gender was 56.1%, which is higher than
that reported as 42% in the Nebraska study (18).
Among KKNG HHC patients circulatory system disorders
mainly stroke (CVA), were the most frequent diagnosis (20.3%),
this goes along with the American study, which showed 23.8%
of the cases being circulatory system disorders. The high
prevalence of circulatory disorders are related to multiple
risk factors i.e. DM, HPN, smoking ...etc.
About 16.2% of the patients studied were diagnosed
to have neoplastic disease similar to 16.9 % reported in the
American study (18). However, in endocrine disorders it was
mainly diabetes at (10.8%). This was higher than what was
reported in the American study, which showed 9.5% of cases
being endocrine disorders (18). Maybe this can be explained
by the higher prevalence of diabetes we have in the Kingdom
of Saudi Arabia.
The American study reported 10.8% of injuries in HHC cases
while the current study showed only 8.8%. The lower percentage
rates maybe a result of the geographical location of the National
Guard Hospital. It is relatively far away and most RTA and
injuries cases referred to other hospitals (i.e. King Fahad
General Hospital). There were no significant differences found
in comparing central system disorders, dermatological, genitourinary,
and bone diseases from those presented by the American study
(18).
The most commons disorders for HHC clients were
the same in both studies (circulatory disorders and neoplasm's).
These results are consistent with the most common causes of
morbidity and moralities. So more efforts need to be done
in the prevention and control of their risk factors. (i.e.
screening for diabetes, hypertension, hyperlipidemia, and
treatment at early stages has to be started). Injuries were
seen more frequently in the age range from 15 years -65 years.
More commonly males are more vulnerable to injuries than females
because they are more active, out doors and plus they are
driving. That is why it is very important that more education
about safety measures during driving and other out door activities
has to be directed to these groups.
For the patients in this study there was 52
(35%) that had other diagnosis's like DM, IHD, and HPN. These
cases were more complex and needed more services for follow
up.
This study showed no significant difference in the length
of hospital stay between HHC patients who were diagnosed to
have CVA and those with CVA and who did not have the home
care services. (14.9 days, 10.6 days for HHC and hospital
cases respectively). The mean numbers of hospital admissions
for HHC patients were lower (0.44) than non-HHC case (0.94)
for hospital CVA patients. This difference has no statistical
significance. This may be due to a small sample size. On the
other hand meta-analysis that reviewed 13 studies showed reduction
of initial hospital stay by 1.7 days and significantly reduced
the total number of hospital days for one year by 2.6 days
per patient with different diagnosis's.(5)
The mean for HHC clinic visits during 6 months
to 1 year was 2 visits. This was lower than non-HHC cases
which mean was 3.3 visits. This difference showed no statistical
significant. However, there was a reduction by approximately
3 visits per patient in other study. (5) The results of the
current study maybe due to a shorter duration of follow up
or cases of CVA needed more care and had more complex problems.
The means for emergency visits in HHC cases
were lower than non-HHC patients (1 visit, 1.4 visits respectively).
But this has no statistical difference, because the same result
was found in other studies previously mentioned. (5) These
results could be affected by small sample size, diagnosis
(CVA) with other complex conditions and by the method of follow
up (patients might be registered in more than one hospital).
On the other hand HHC patient may stick to KKNGH because of
its HHC service. Other studies done on HHC CVA cases showed
interesting sides of the issue that have not been studied
in the current study. Thus Two studies done on CVA patients
who are receiving home care showed an increase in the patient
and carer satisfaction. (20) Also anther study showed that
adverse outcome was less in CVA patients receiving home therapy.
(21)

REFERENCES
- Montauk, S. L. Home Health
Care. American Family Physician 1998; 58:1608- 1614.
- Linda N. Meurer, M.D,
M.P.H, John R. Meurer, M.D., M.M., and Richard Holloway,
Ph.D. Home New Models of Health Care
in the home and in the Work Site. American Family Physician
August 1997; 56:
- Ian R. Mcwhinney, M.D.,F.R.C.G.P.A
Textbook of Family Medicine, 2nd Edition Ian R. McWhinney,
M.D., F.R.C.G.P., F.C.F.P., F.R.C.P. Professor Emeritus,
Department of Family Medicine., University of Western Ontario
- Home Care by Lawrence
H. Bernstein
- How to get the most benefit
from a changing home health care system Appavuchetty Soundappan,
MD Terry Goodwin, MA, RN Roberta Greengold, MS, MBA, RN
Eugenia L. Siegler, MD
- Saudi Arabia: The Kingdom,
Its Health Care Programs, and the Beginning of Home Health
Care by Peggy L. Galloway, RN.
- Annals of Saudi Medicine,
Vol. 15, No. 4,1995. Developing Palliative Care Services
for Terminally Ill patients in Saudi Arabia, by Alan J.
Gray, MB, ChB, FRACP, FRACR: Adnan Ezzat, MB, BCh, FRCPC:
Susan Volker, BSN, MPH.
- Jeddah Today 1994. Published
by: Jeddah Chamber of Commerce & Industry P.O. Box:
1264, Jeddah 21431, Saudi Arabia.
- William R. Phillips. Building the Future
of Health Care on the Foundations of Family Practice. Family
Practice Management, Jan 2000. Am Aca Fam Phy (AAFP).
- Ramsdell SW, Swart J,
Jackson JE, Renvall M. The yield of home visit in the assessment
of geriatric patients. J Am Geriatr Soc, 1989; 37: 17-24.
- Tideikaar R. Environmental
adoptation to preserve balance and prevent fall. Top Geriatr
Rehabil 1990; S 178-84.
- Unwin BK, Jerant AF. The
home visit. American Family Physician., 1999(Oct.1). Am
Aca Fam Phy (AAFP.
- Freeman SR, Chambers KA.
Home Health Care: Clinical pathways and quality integration.
Nursing Management, June 1997; 28(6): 45-48.
- Melin AL, Hakansson S,
Bygren LO. The cost effectiveness of rehabilitation in the
home: A study of Swedish elderly. Am J Pub Health, Mar 1993;
83(3): 356-362.
- Stuck AE, Aronow HU, Steiner
A, Alessi CA, Bula CJ, Gold MN, Yuhas KE et al. A trial
of annual in home comprehensive geriatric assessments for
elderly people living in the community. The New England
Journal of Medicine (NEJM), 1995(Nov 2); 333(18): 1184-89.
- Intrator O, Berg K. Benefits
of Home Health Care after inpatient rehabilitation for hip
fracture: Health service use by medicare beneficiaries,
1987-1992. Arch Phys Med Rehabil 1998 (Oct.); 79: 1195-1199.
- Mostafa M. Elhilali. Early
hospital discharge and home care. Canadian Journal of Surgery
1997(Feb.);4.
- Gijn JV, Dennis MS. Issues
and Answers in Stroke Care. Lancet 1998 (Oct. 24); 352:
(Suppl II) 23-27.
- Shepperd S, Lliffe S. Hospital-at-home versus
in-patient hospital care. The Cochrane Library, (1) 2000;
Oxford: Update Software.20.
- Martin KS, Scheet NJ, Stegman MR. Home Health
Clients: Characteristics, Outcomes of Care, and Nursing
Interventions. Am J Pub Health 1993 (Dec.); 83 (12): 1730-1734
|








